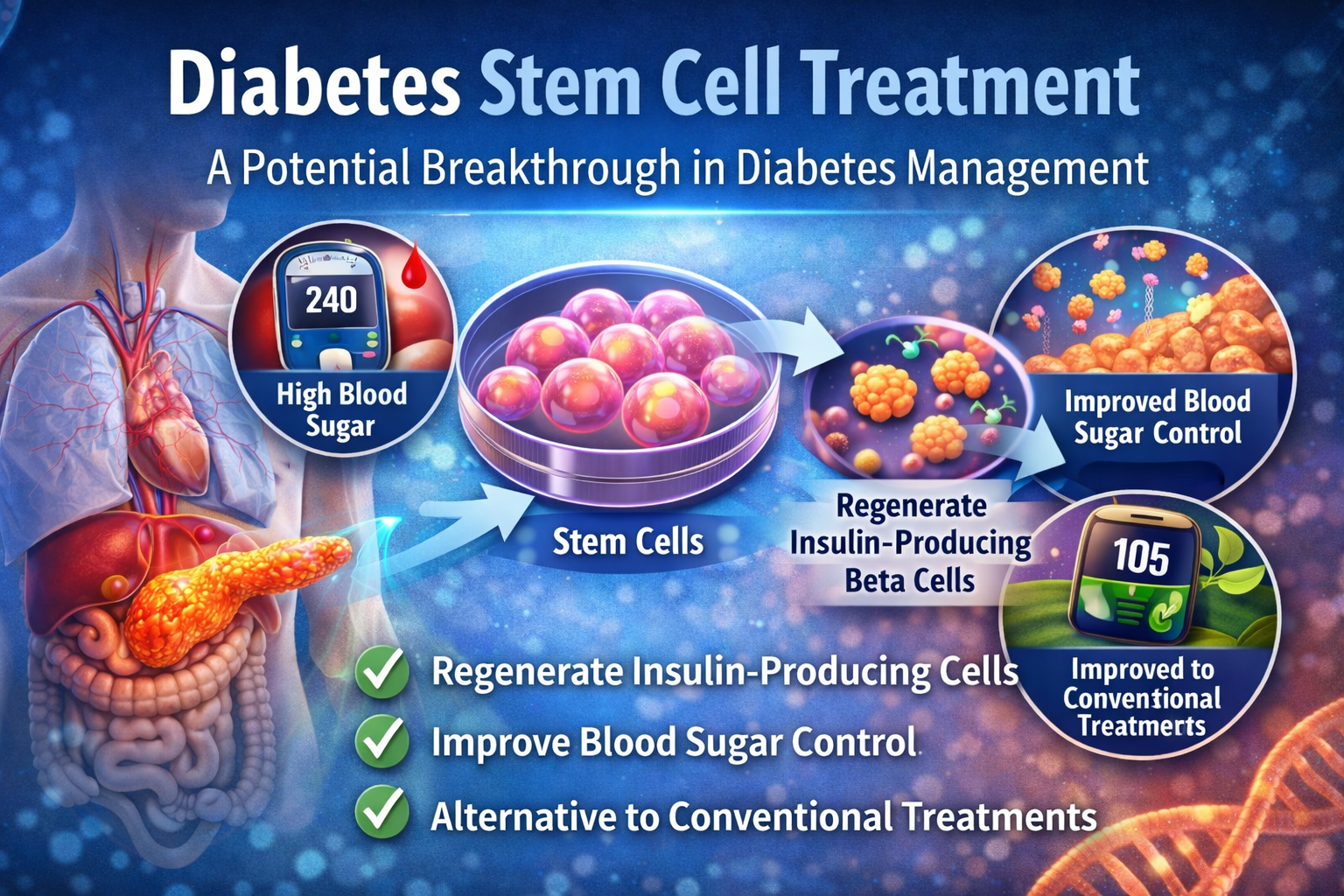
A Guide to Diabetes Stem Cell Treatment and Its Potential Benefits
Diabetes is one of the most common chronic health conditions affecting millions of people worldwide. It occurs when the body cannot properly regulate blood sugar levels due to problems with insulin production or insulin use. Over the years, medical science has explored many ways to manage this condition. One emerging area of research is Diabetes Stem Cell Treatment, which is gaining attention for its potential to improve how the body handles blood glucose.
Understanding Diabetes
Diabetes is generally classified into two main types: Type 1 and Type 2. Type 1 occurs when the immune system attacks the insulin-producing cells in the pancreas. As a result, the body cannot produce insulin, a hormone necessary for controlling blood sugar levels. Type 2 diabetes is more common and develops when the body becomes resistant to insulin or does not produce enough of it.
Traditional management usually includes medication, insulin therapy, regular monitoring of blood glucose, physical activity, and dietary adjustments. These methods help control symptoms and reduce complications. However, they do not fully restore the damaged cells responsible for insulin production. This limitation has led researchers to investigate regenerative medical approaches.
What Are Stem Cells?
Stem cells are special cells that have the ability to develop into different types of cells in the body. They can also repair or replace damaged tissues. Because of these unique properties, stem cells are widely studied in regenerative medicine for conditions involving cell damage or degeneration.
These cells can be obtained from several sources, including bone marrow, adipose tissue (fat), and umbilical cord tissue. Scientists believe that stem cells may help regenerate pancreatic cells that produce insulin. This idea has encouraged ongoing research into Diabetes Stem Cell Treatment as a possible supportive therapy for diabetes management.
How Stem Cells May Help in Diabetes
The concept behind stem cell therapy is based on the regeneration of pancreatic beta cells. These cells are responsible for producing insulin in the body. When these cells become damaged or destroyed, blood sugar levels rise.
In theory, stem cells introduced into the body may help repair or regenerate these insulin-producing cells. In addition to cell regeneration, stem cells may also support immune system regulation and reduce inflammation. These effects could potentially improve how the body responds to insulin.
Scientists are still working to fully understand how these cells behave after being introduced into the body. Clinical studies continue to explore whether stem cell therapies can offer long-term benefits for individuals with diabetes.
The Treatment Process
The procedure for stem cell therapy usually involves several stages. First, doctors evaluate the patient’s medical history, overall health, and the severity of the condition. This step ensures that the individual is suitable for the therapy.
Once eligibility is confirmed, stem cells are collected from an approved source. After processing in specialized laboratories, the cells are introduced into the body through intravenous infusion or targeted injection. The goal is to allow the cells to travel to damaged tissues and support natural healing processes.
After treatment, patients are typically monitored through follow-up visits and medical tests. These evaluations help doctors observe how the body responds to the therapy and whether improvements occur in blood sugar control.
Potential Benefits Being Studied
Research suggests that regenerative therapies may offer several potential advantages. Although results can vary from patient to patient, the following areas are often studied in clinical trials:
-
Support for pancreatic cell repair
-
Improved insulin sensitivity
-
Better blood sugar stability
-
Reduced dependence on external insulin in some cases
-
Support for overall metabolic function
It is important to note that many of these outcomes are still under investigation. Medical experts emphasize that stem cell therapies are part of ongoing research and may not replace conventional diabetes treatments.
Safety and Medical Considerations
As with any medical procedure, safety is a key concern. Stem cell therapy should always be performed in licensed medical facilities under the supervision of experienced specialists. Proper screening and laboratory standards are essential to ensure the quality and safety of the cells used.
Patients considering Diabetes Stem Cell Treatment should consult qualified healthcare professionals before making decisions. Doctors can explain potential benefits, limitations, and possible risks based on the patient’s specific medical condition.
Regulatory authorities in different countries also set guidelines for the use of stem cells in clinical practice. These regulations help ensure that treatments follow established medical and ethical standards.
Current Research and Future Possibilities
Scientists around the world continue to explore new ways to use stem cells in diabetes care. Researchers are studying different types of stem cells, including mesenchymal stem cells and induced pluripotent stem cells. These cells may offer different regenerative capabilities and could lead to improved therapies in the future.
Another area of research focuses on protecting newly formed pancreatic cells from immune system attacks. This is particularly important for people with Type 1 diabetes, where the immune system destroys insulin-producing cells. If scientists can prevent this immune response, regenerative therapies could become more effective.
Technological advancements in cell engineering and laboratory techniques are also accelerating progress. While these developments are promising, more long-term clinical studies are required to confirm their safety and effectiveness.
Lifestyle Still Plays an Important Role
Even with new medical technologies, lifestyle management remains a critical part of diabetes care. Healthy eating, regular physical activity, and routine medical monitoring continue to be essential for maintaining stable blood sugar levels.
Patients who explore advanced therapies should still follow the guidance of their healthcare providers regarding diet, medication, and daily habits. Combining medical treatments with a balanced lifestyle can help support overall well-being.
Conclusion
Advances in regenerative medicine are opening new possibilities in the field of diabetes management. Stem cell research offers hope for repairing or supporting the body’s natural insulin-producing abilities. While the science continues to develop, Diabetes Stem Cell Treatment is being studied as a promising approach that may complement traditional therapies.
People interested in this form of treatment should seek professional medical advice and learn about the latest research and clinical options available. With continued scientific progress, regenerative medicine may play a greater role in improving the lives of individuals living with diabetes in the future.